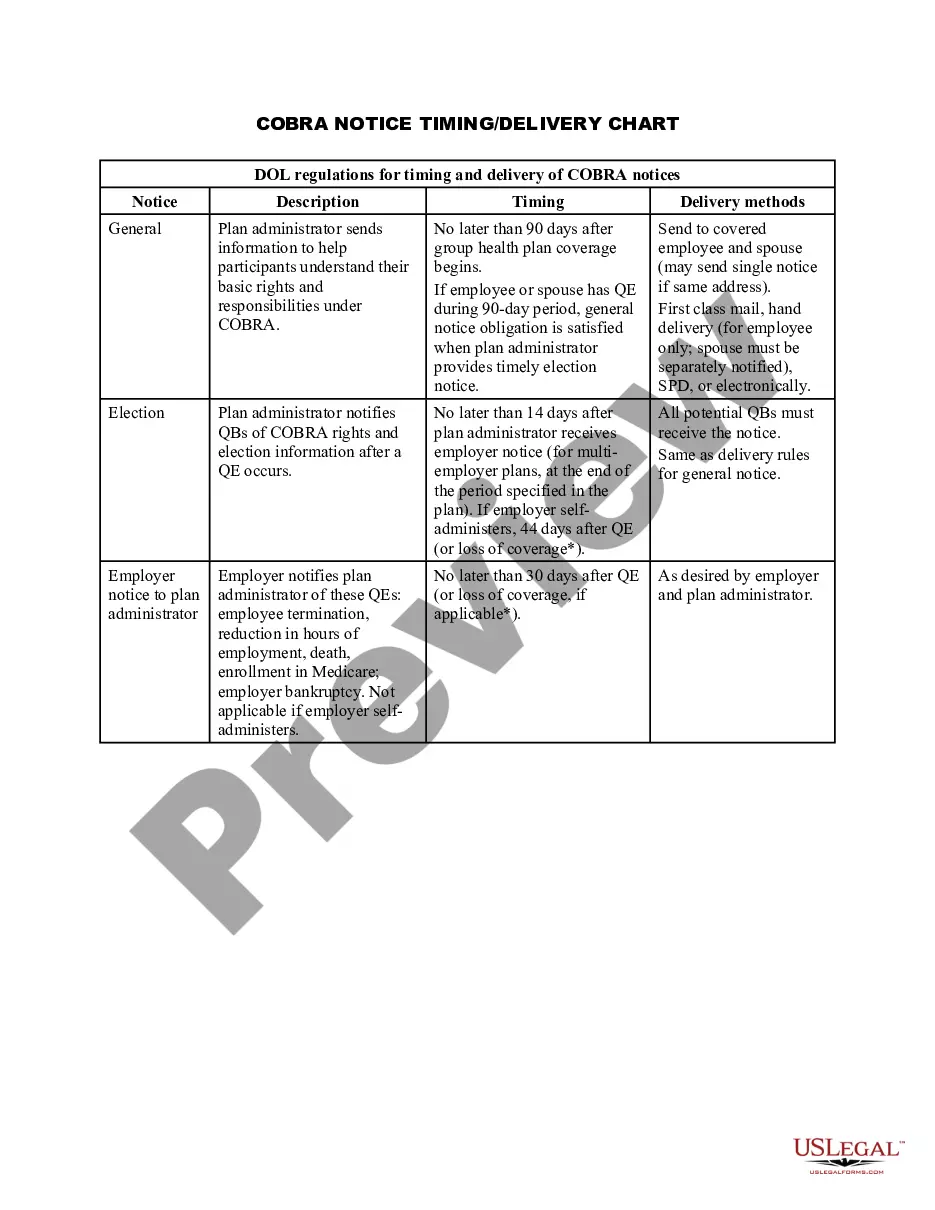
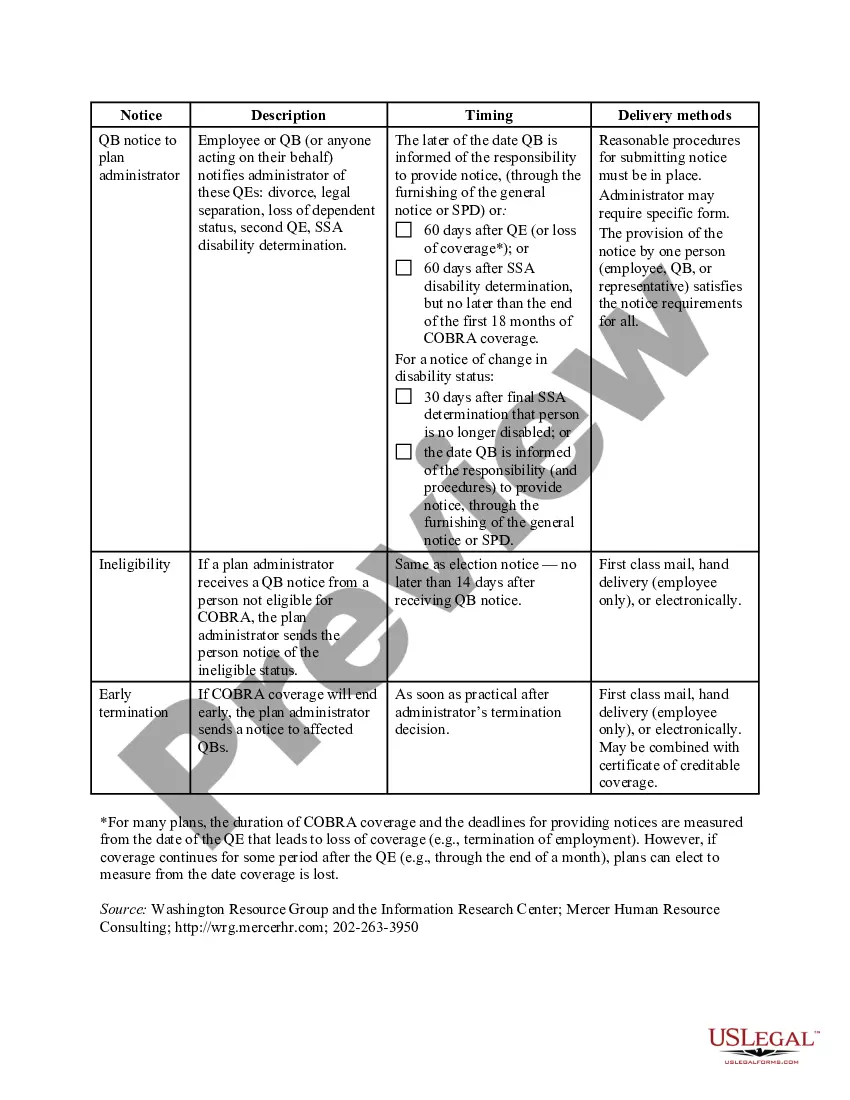
Maryland COBRA Notice Timing Delivery Chart is a vital resource for employers and employees in the state of Maryland to ensure compliance with COBRA (Consolidated Omnibus Budget Reconciliation Act) notice timing requirements. COBRA provides eligible employees and their dependents with the opportunity to continue health insurance coverage after a qualifying event such as termination, reduction in hours, or divorce. This comprehensive chart outlines the specific timeframes within which various COBRA notices must be delivered to employees and beneficiaries. It serves as a valuable reference tool for employers, human resources professionals, and benefits administrators, ensuring that they adhere to the legal obligations of timely COBRA notice delivery. The Maryland COBRA Notice Timing Delivery Chart includes the following types of notices: 1. Initial Notice: This notice, also known as the General Notice, is provided to an employee and their covered dependents within 90 days from the date they became eligible for COBRA coverage. It explains the rights and responsibilities of the individuals and provides details about the COBRA continuation coverage options available. 2. Qualifying Event Notice: Employers must provide this notice within 30 days of a qualifying event, such as termination, reduction in hours, or divorce. It informs the affected employee and qualified beneficiaries about their COBRA rights and the steps they need to take to continue their health insurance coverage. 3. Election Notice: Once a qualifying event occurs, this notice must be delivered within 14 days to the affected individual. It includes information about the COBRA coverage options, premium costs, and the timeframe for making an election to continue coverage. 4. Notice of Unavailability of COBRA Coverage: If an individual is not eligible for COBRA continuation coverage, this notice must be sent promptly but no later than 14 days after the determination of ineligibility. It explains the reasons behind the ineligibility and may suggest alternative coverage options. The Maryland COBRA Notice Timing Delivery Chart helps employers avoid potential legal penalties and ensures that employees and beneficiaries have access to critical healthcare coverage information. It is crucial to consult this chart and strictly adhere to the timeframes mentioned to facilitate a smooth transition between employer-sponsored health insurance plans. Keywords: Maryland, COBRA, Notice, Timing, Delivery, Chart, COBRA Notices, Compliance, Eligible employees, Qualifying event, Initial Notice, General Notice, Qualifying Event Notice, Election Notice, Notice of Unavailability of COBRA Coverage, Legal obligations, Health insurance coverage, Benefits administrators, Human resources professionals, Timely delivery.
Maryland COBRA Notice Timing Delivery Chart
Description
How to fill out Maryland COBRA Notice Timing Delivery Chart?
US Legal Forms - one of many biggest libraries of authorized types in the States - gives an array of authorized record layouts you are able to download or printing. Utilizing the web site, you can find 1000s of types for company and individual uses, sorted by groups, states, or keywords.You will discover the latest models of types much like the Maryland COBRA Notice Timing Delivery Chart within minutes.
If you currently have a monthly subscription, log in and download Maryland COBRA Notice Timing Delivery Chart through the US Legal Forms catalogue. The Obtain option can look on every type you look at. You have accessibility to all previously acquired types in the My Forms tab of your profile.
In order to use US Legal Forms for the first time, here are straightforward recommendations to help you get began:
- Be sure to have picked out the best type for your area/region. Click on the Review option to check the form`s articles. Look at the type outline to actually have selected the correct type.
- In case the type doesn`t match your demands, take advantage of the Search area towards the top of the monitor to find the one which does.
- Should you be satisfied with the form, affirm your decision by clicking the Acquire now option. Then, pick the costs prepare you favor and supply your qualifications to register for an profile.
- Procedure the transaction. Make use of credit card or PayPal profile to accomplish the transaction.
- Find the format and download the form on the product.
- Make adjustments. Fill out, modify and printing and sign the acquired Maryland COBRA Notice Timing Delivery Chart.
Every single web template you included in your account does not have an expiry time and is also your own eternally. So, if you wish to download or printing another duplicate, just check out the My Forms segment and click on in the type you will need.
Obtain access to the Maryland COBRA Notice Timing Delivery Chart with US Legal Forms, the most extensive catalogue of authorized record layouts. Use 1000s of professional and state-certain layouts that satisfy your company or individual requires and demands.