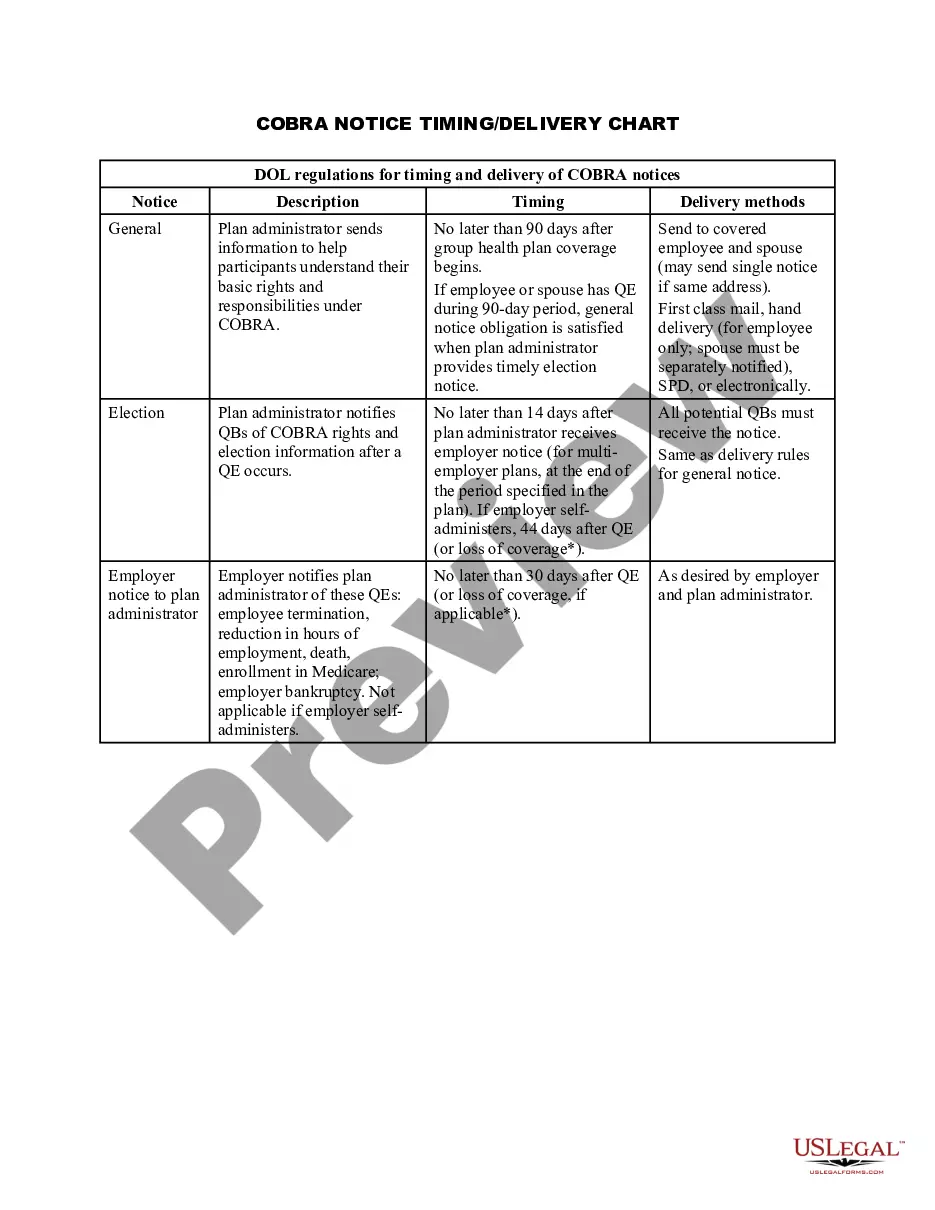
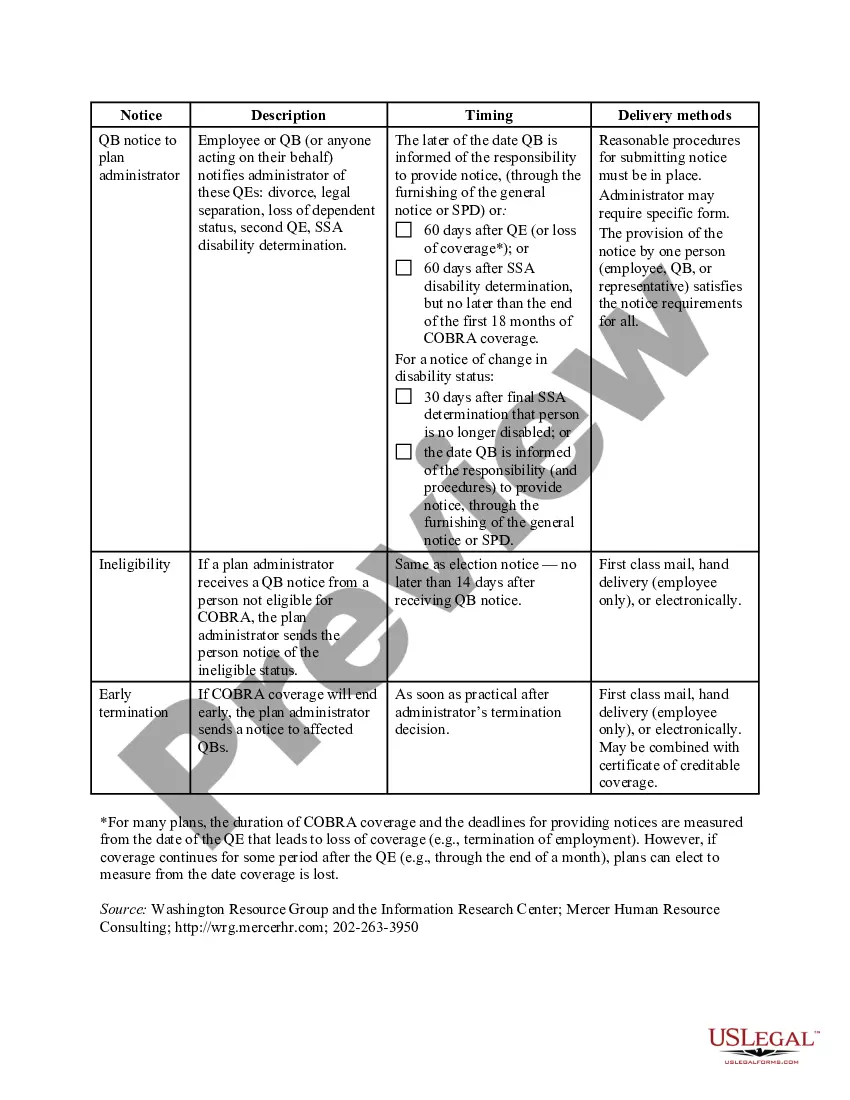
The Texas COBRA Notice Timing Delivery Chart is a comprehensive guide that outlines the specific deadlines and timelines for delivering COBRA notices to eligible individuals in the state of Texas. This chart serves as a reliable resource for employers and healthcare plan administrators to ensure compliance with COBRA regulations and avoid penalties. The timing of COBRA notice delivery is of utmost importance to provide eligible individuals with the necessary information and options regarding their continuation of healthcare coverage. Failure to comply with the specified deadlines outlined in the Texas COBRA Notice Timing Delivery Chart may result in legal repercussions and financial liabilities. The chart categorizes the various types of COBRA notice delivery and their respective timeframes. These may include: 1. General COBRA Initial Notice: This is the initial notice that must be provided to all covered employees and their dependents within 90 days of their health coverage's commencement. It highlights the individual's rights and responsibilities under COBRA, including the option to continue healthcare coverage after experiencing a qualifying event. 2. Qualifying Event Notice: Following a qualifying event such as termination, reduction in work hours, or divorce, this notice should be sent to the covered individual and their eligible dependents within 14 days of the employer's knowledge of the event. It informs them of their right to elect COBRA coverage and provides the necessary information to do so. 3. Notice of Unavailability: If the employer is unable to offer COBRA coverage due to plan termination or other reasons, this notice needs to be delivered within a reasonable period but no later than 30 days after the employer's knowledge of the unavailability. It informs eligible individuals of alternative coverage options that they may pursue. 4. Conversion Notice: In cases where COBRA coverage is not available due to exceptional circumstances, such as bankruptcy or loss of group coverage eligibility, the conversion notice must be disseminated within 15 days of the employer's knowledge of ineligibility. It provides information regarding the possibility of converting group coverage to an individual policy. The Texas COBRA Notice Timing Delivery Chart incorporates all the essential deadlines and timelines required for each type of notice, ensuring that employers and healthcare plan administrators stay compliant with COBRA regulations in the state. By adhering to these guidelines, employers can fulfill their obligations and avoid potential legal issues related to COBRA notice delivery.
Texas COBRA Notice Timing Delivery Chart
Description
How to fill out Texas COBRA Notice Timing Delivery Chart?
Are you presently inside a situation where you need paperwork for both enterprise or person uses almost every working day? There are a variety of legal document web templates available on the net, but getting ones you can depend on isn`t effortless. US Legal Forms delivers a large number of develop web templates, like the Texas COBRA Notice Timing Delivery Chart, that are published in order to meet federal and state demands.
Should you be presently knowledgeable about US Legal Forms website and possess your account, just log in. Following that, you may down load the Texas COBRA Notice Timing Delivery Chart format.
Unless you have an accounts and need to begin to use US Legal Forms, abide by these steps:
- Obtain the develop you want and make sure it is for that right area/area.
- Make use of the Review switch to review the shape.
- See the outline to actually have selected the appropriate develop.
- If the develop isn`t what you are trying to find, take advantage of the Research area to get the develop that fits your needs and demands.
- When you find the right develop, just click Get now.
- Choose the rates plan you desire, complete the required information and facts to create your bank account, and pay for your order using your PayPal or credit card.
- Decide on a hassle-free data file formatting and down load your duplicate.
Discover each of the document web templates you may have bought in the My Forms menus. You may get a additional duplicate of Texas COBRA Notice Timing Delivery Chart anytime, if possible. Just select the needed develop to down load or printing the document format.
Use US Legal Forms, by far the most substantial selection of legal forms, in order to save efforts and stay away from mistakes. The support delivers expertly made legal document web templates which you can use for a selection of uses. Generate your account on US Legal Forms and begin generating your daily life a little easier.