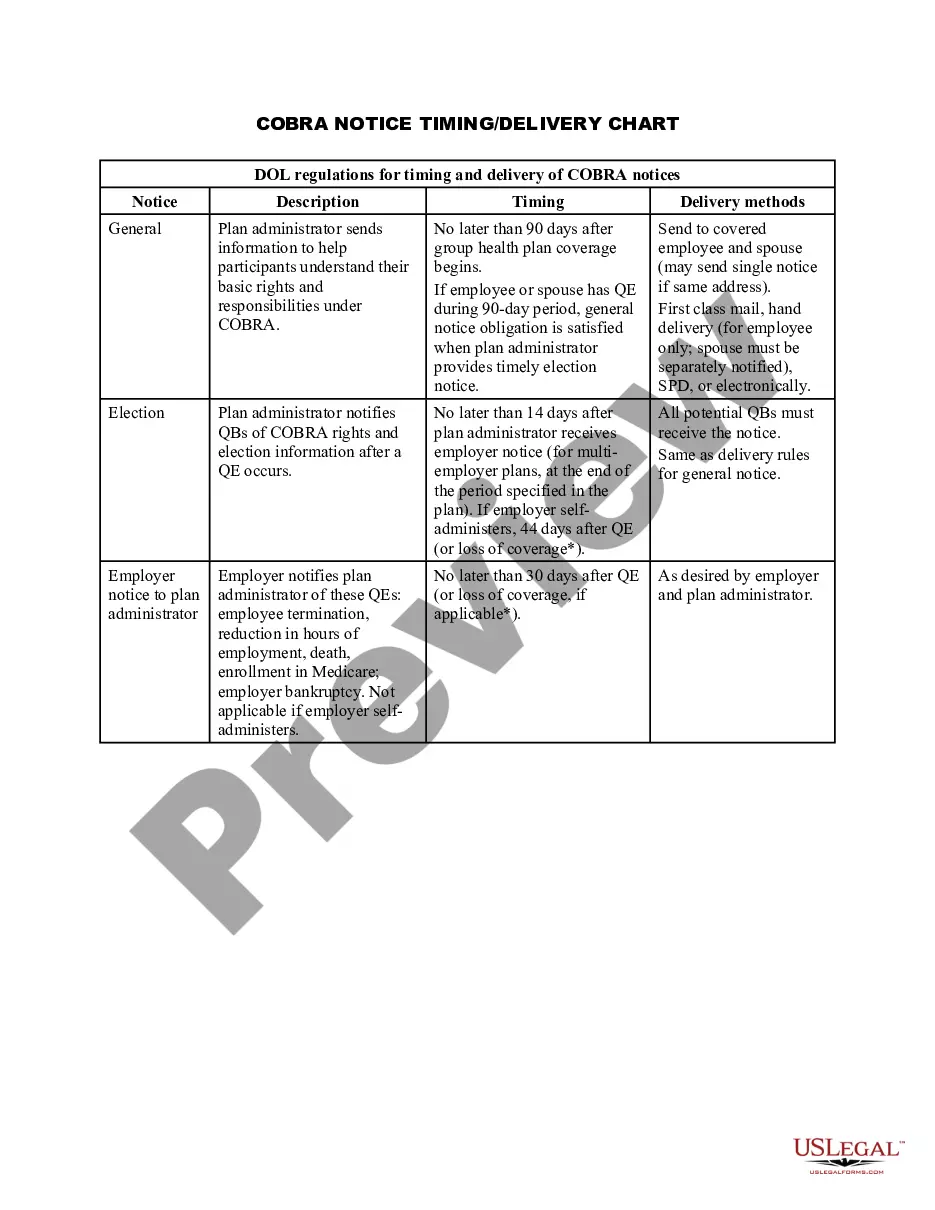
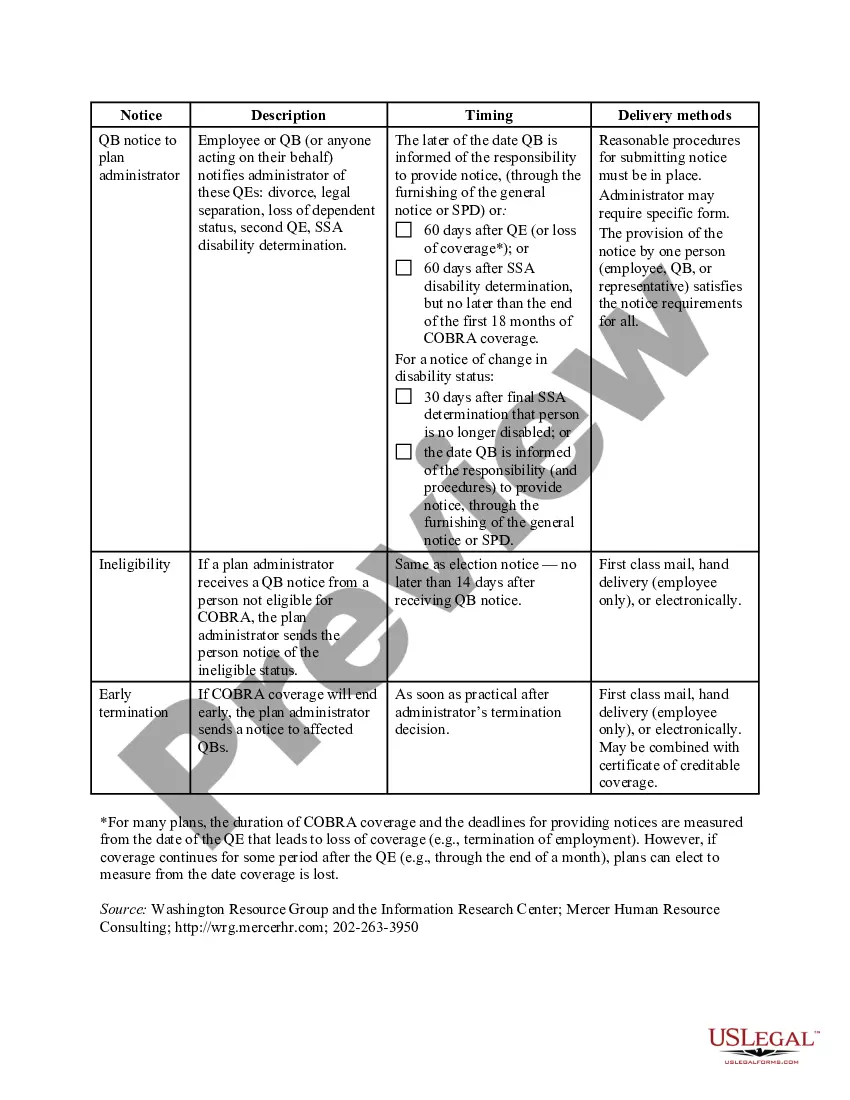
The Contra Costa California COBRA Notice Timing Delivery Chart is an essential reference tool designed to provide important information regarding COBRA notice timelines in Contra Costa County, California. COBRA, which stands for Consolidated Omnibus Budget Reconciliation Act, is a federal law that allows employees and their dependents to maintain health insurance coverage for a limited time after experiencing qualifying events such as job loss or reduction in work hours. The COBRA Notice Timing Delivery Chart serves as a comprehensive guide outlining the required timeframe for delivering COBRA notices to eligible individuals. It ensures compliance with the COBRA regulations and helps employers and health plan administrators avoid penalties and legal issues related to non-compliance. This informative chart encompasses various types of COBRA notice delivery timelines to accommodate different circumstances. It includes: 1. Initial COBRA Notice: This notice must be provided to qualified employees and their dependents within 90 days of their health plan's commencement or the qualifying event that triggered their eligibility for COBRA continuation coverage. 2. General Notice: The general notice is a comprehensive document explaining COBRA benefits, rights, and obligations. It must be distributed to all employees and their dependents within the first 90 days of coverage under the health plan. 3. Qualifying Event Notice: In case of a qualifying event, such as termination, reduction in hours, or divorce, a notice must be sent within 14 days to the covered employee or the plan administrator, whichever is responsible for providing the notice. 4. Election Notice: The election notice must be provided to the qualified beneficiaries within 14 days after the plan administrator receives the notice of a qualifying event. This notice outlines the available coverage options, costs, and the deadline for enrolling in COBRA continuation coverage. 5. Notice of Unavailability: If an individual is deemed ineligible for COBRA continuation coverage, a notice that explains the reason for ineligibility should be delivered within 14 days after receiving the notice of a qualifying event. By adhering to the Contra Costa California COBRA Notice Timing Delivery Chart, employers and health plan administrators can ensure timely and accurate delivery of essential information to eligible individuals, facilitating their access to continued healthcare coverage during challenging times. Compliance with COBRA regulations not only protects the interests of employees and their dependents but also helps employers maintain legal compliance and mitigate potential legal risks associated with non-compliance. Employers and health plan administrators must remain vigilant in staying up-to-date with the latest COBRA regulations and adjusting their notice delivery processes accordingly to ensure full compliance with the law. The Contra Costa California COBRA Notice Timing Delivery Chart serves as a valuable resource for the accurate management of COBRA notices, promoting transparency and accountability in providing continued health coverage options for eligible individuals.
Contra Costa California COBRA Notice Timing Delivery Chart
Description
How to fill out Contra Costa California COBRA Notice Timing Delivery Chart?
How much time does it typically take you to create a legal document? Considering that every state has its laws and regulations for every life scenario, finding a Contra Costa COBRA Notice Timing Delivery Chart suiting all local requirements can be stressful, and ordering it from a professional lawyer is often expensive. Many online services offer the most popular state-specific templates for download, but using the US Legal Forms library is most advantegeous.
US Legal Forms is the most extensive online collection of templates, collected by states and areas of use. In addition to the Contra Costa COBRA Notice Timing Delivery Chart, here you can find any specific document to run your business or individual affairs, complying with your county requirements. Specialists verify all samples for their actuality, so you can be certain to prepare your paperwork correctly.
Using the service is remarkably straightforward. If you already have an account on the platform and your subscription is valid, you only need to log in, choose the needed sample, and download it. You can pick the file in your profile anytime later on. Otherwise, if you are new to the platform, there will be some extra steps to complete before you obtain your Contra Costa COBRA Notice Timing Delivery Chart:
- Examine the content of the page you’re on.
- Read the description of the template or Preview it (if available).
- Search for another document utilizing the related option in the header.
- Click Buy Now once you’re certain in the selected file.
- Decide on the subscription plan that suits you most.
- Create an account on the platform or log in to proceed to payment options.
- Pay via PalPal or with your credit card.
- Switch the file format if necessary.
- Click Download to save the Contra Costa COBRA Notice Timing Delivery Chart.
- Print the doc or use any preferred online editor to complete it electronically.
No matter how many times you need to use the acquired document, you can find all the files you’ve ever saved in your profile by opening the My Forms tab. Give it a try!