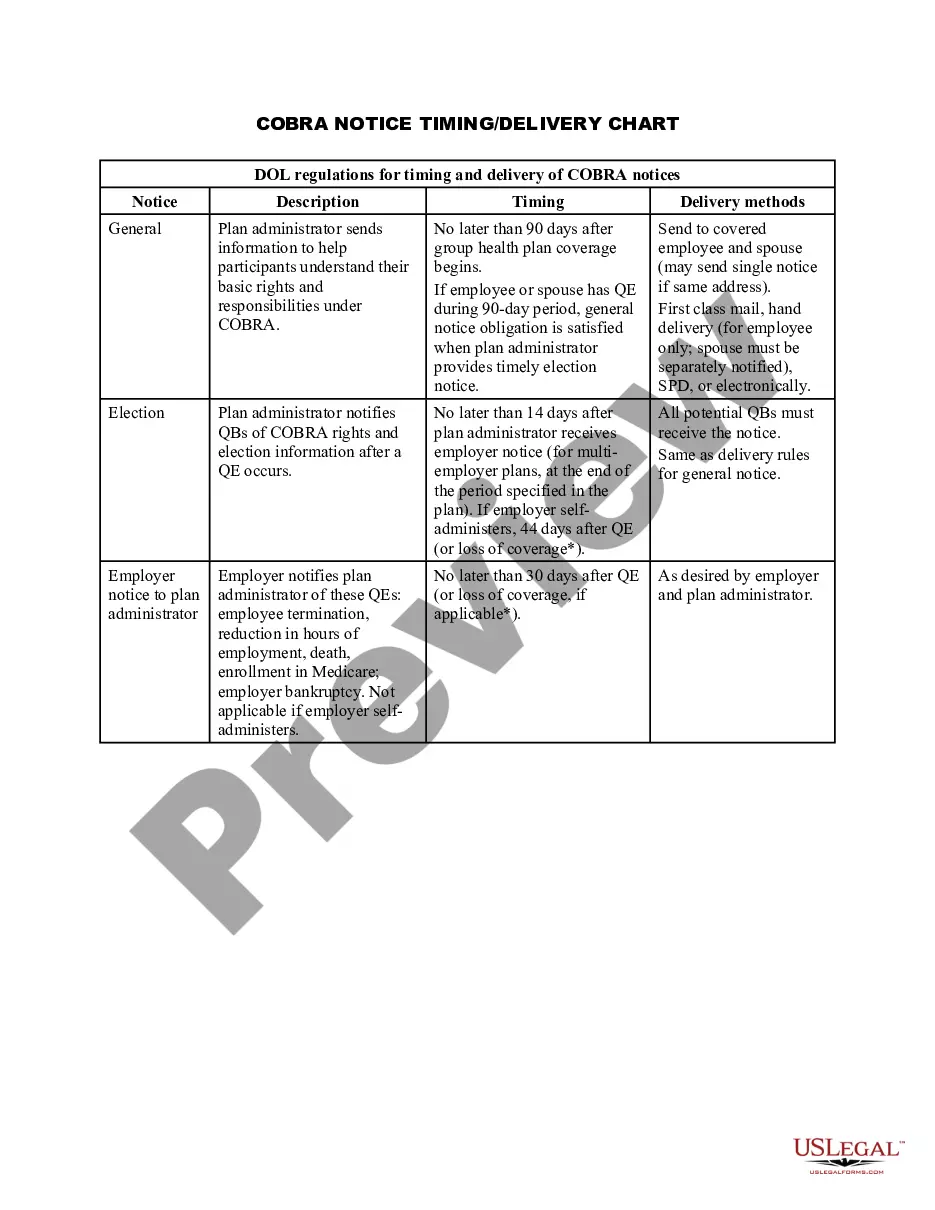
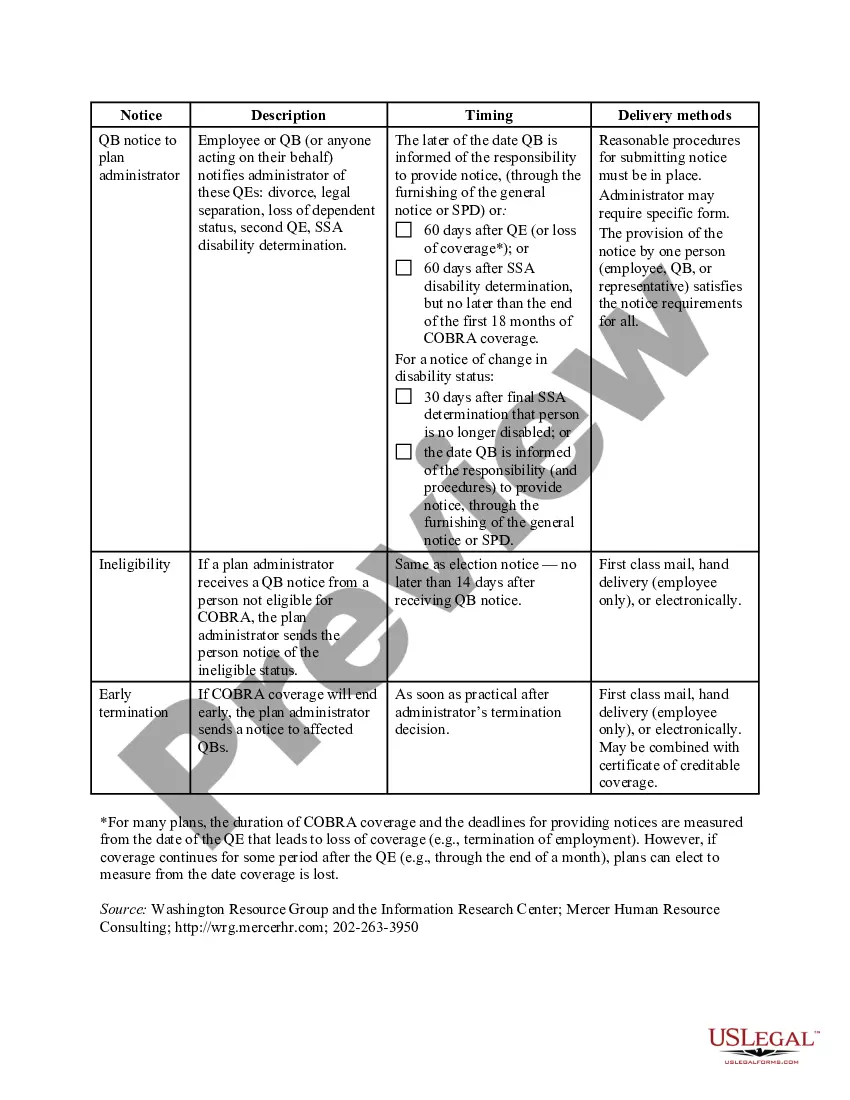
The Middlesex Massachusetts COBRA Notice Timing Delivery Chart is a crucial resource that provides detailed information regarding the delivery timelines associated with COBRA (Consolidated Omnibus Budget Reconciliation Act) notices in Middlesex County, Massachusetts. COBRA is a federal law that allows employees and their dependents to continue their group health insurance coverage, even after their employment has ended or certain qualifying events have occurred. The COBRA Notice Timing Delivery Chart for Middlesex County outlines the specific timeframes within which employers must provide various COBRA notices to their employees and beneficiaries. These notices serve to inform individuals of their rights to continue their health insurance coverage and explain the necessary steps for enrollment and payment. Compliance with the timing requirements outlined in the chart is essential to ensure that employees and dependents have adequate time to make informed decisions about their healthcare coverage options. The Middlesex Massachusetts COBRA Notice Timing Delivery Chart covers various types of COBRA notices, including: 1. General COBRA Initial Notice: This notice is typically distributed to all covered employees and their dependents within 90 days from the coverage's start date. It outlines the rights and responsibilities under COBRA, including the timeframe for electing continuation coverage. 2. Qualifying Event Notices: These notices are sent when certain qualifying events, such as termination of employment, reduction of hours, or divorce, occur. Both the employer and the qualified beneficiary must provide timely notification to the plan administrator within specific timeframes as per the chart guidelines. 3. COBRA Election Notice: This notice provides individuals with the opportunity to elect continuation coverage within the stipulated timeframe after receiving the Qualifying Event Notice. It includes details on the coverage options available, applicable premiums, and the deadline for submitting the election form. 4. Notice of Unavailability of Continuation Coverage: In some cases, employers may determine that COBRA continuation coverage is not available to certain individuals who would otherwise be eligible. This notice must be provided promptly, explaining the reasons for ineligibility and providing information on alternative coverage options. 5. Notice of Early Termination: Under certain circumstances, an employer's obligation to provide COBRA coverage may end prematurely. The Notice of Early Termination informs qualified beneficiaries about the cessation of coverage before the originally specified end date. By referring to the Middlesex Massachusetts COBRA Notice Timing Delivery Chart, employers can ensure compliance with COBRA notice requirements and guarantee that employees and their dependents have adequate time to understand their rights and make informed decisions about their health insurance coverage.
Middlesex Massachusetts COBRA Notice Timing Delivery Chart
Description
How to fill out Middlesex Massachusetts COBRA Notice Timing Delivery Chart?
A document routine always goes along with any legal activity you make. Opening a business, applying or accepting a job offer, transferring property, and many other life situations require you prepare official documentation that differs from state to state. That's why having it all collected in one place is so helpful.
US Legal Forms is the largest online library of up-to-date federal and state-specific legal forms. Here, you can easily find and download a document for any personal or business objective utilized in your region, including the Middlesex COBRA Notice Timing Delivery Chart.
Locating templates on the platform is remarkably straightforward. If you already have a subscription to our library, log in to your account, find the sample using the search bar, and click Download to save it on your device. Afterward, the Middlesex COBRA Notice Timing Delivery Chart will be available for further use in the My Forms tab of your profile.
If you are using US Legal Forms for the first time, adhere to this simple guideline to get the Middlesex COBRA Notice Timing Delivery Chart:
- Ensure you have opened the proper page with your regional form.
- Use the Preview mode (if available) and scroll through the template.
- Read the description (if any) to ensure the template corresponds to your requirements.
- Search for another document using the search tab if the sample doesn't fit you.
- Click Buy Now once you find the required template.
- Decide on the suitable subscription plan, then log in or register for an account.
- Select the preferred payment method (with credit card or PayPal) to continue.
- Opt for file format and save the Middlesex COBRA Notice Timing Delivery Chart on your device.
- Use it as needed: print it or fill it out electronically, sign it, and send where requested.
This is the simplest and most reliable way to obtain legal paperwork. All the samples provided by our library are professionally drafted and verified for correspondence to local laws and regulations. Prepare your paperwork and run your legal affairs properly with the US Legal Forms!